Different tests for COVID-19 explained
June 15, 2020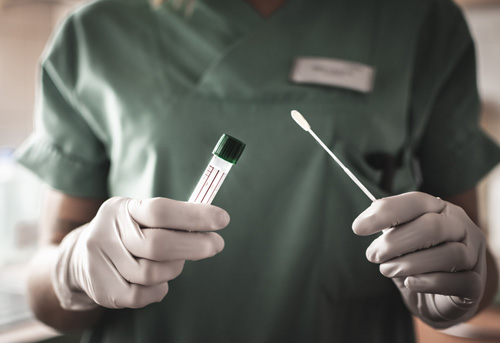
Different tests for COVID-19 explained
by Dr. Tom Bracken
Mille Lacs Health System
Like most aspects of our COVID virus epidemic, there has been a lot of confusion regarding COVID tests. There are three main tests for the COVID virus infection.
The first test is the PCR test. PCR stands for Polymerase Chain Reaction that detects viral proteins. This test takes two to four days to be processed.
This test is done from a specimen from a swab put into your nose to touch the high portion of your throat. The test checks for the presence of specific virus RNA from the COVID-19 virus; it does not tell you whether that virus is still active or whether you are actually ill from it. The test becomes positive about a week after you first contract the virus, which is also about the time you usually first have symptoms. We know that some patients never develop symptoms so you can have a positive test but have no symptoms.
The PCR test remains positive for about three to four weeks after onset of illness and then becomes negative. A positive test after full recovery does not necessarily mean a person is still infective. No test is perfect, and it is thought that this test is somewhere near 95% accurate because samples may be insufficient, etc.
The second test, similar to the PCR test is the so-called “rapid test.” This is also obtained with a swab. Abbott company has developed the most widely used test; it uses isonuclear acid amplification technology to detect viral molecules. Results are available in about 15 minutes. The downside to the rapid test is that it is thought to be less accurate (75%), with more tests reported falsely negative. If it is positive, it is likely truly positive.
The third type of testing for COVID-19 is antibody testing, also known as “serology.” This tests for whether or not you have developed antibodies to COVID-19. These antibodies usually start to develop about the second or third week of infection and are usually positive by week four. This test is thought to be highly specific with a low probability of reporting positive without really having had COVID-19.
The purpose of that test would be to tell you that you have had the disease in the past. The test is usually not positive during the earlier and more severe stages of the illness.
We have not seen patients with positive antibodies get the illness twice; however, the virus could mutate with time, so having a positive antibody test does not guarantee immunity.
We now have all three of these tests available at Mille Lacs Health System. However, our supply remains limited as regards the PCR and rapid tests. Thus we are limiting their use to higher risk patients that fall into certain categories.
We are fortunate that our peak time for illness will be late here compared to many other states – hopefully we will have more tests available then.
